|
When I think of a sit-up, my mind flashes immediately to the (carpeted, for some reason) floor of my elementary-school gym. Twice a week, our teachers marched us there for ritual humiliation and light calisthenics, and under the watchful gaze of a former football coach with a whistle perpetually dangling from his lips, we’d warm up with the moves we’d been told were the building blocks of physical fitness—jumping jacks, push-ups, toe touches, and, of course, sit-ups. With rare exception, we were bad at sit-ups. We’d try our best, taking turns leaning on our partners’ toes as they threw their torsos up and forward for a count of 10. But kids are floppy creatures, and sit-ups are an especially floppy exercise. In gym class, our lower backs hunched, our necks strained, and our arms flew away from their cross-chest Dracula pose. Once a year, beginning in elementary school, the Presidential Fitness Test required us to do as many sit-ups in a minute as our little bodies could stand. Eventually we were introduced to crunches, a truncated variation of the sit-up that made our by-then-adolescent flailing a bit less dramatic. The idea behind those lessons had been the same for generations: Doing sit-ups or crunches at a high volume is not just a reliable way to build physical strength, but a reliable way to measure it. As both a unit of exercise and a way of life, the sit-up was endorsed by the only kinds of fitness experts most people had access to at the time—gym teachers, my exercise-nut dad, the hardbodies in 1990s fitness informercials hawking questionably efficacious gadgets such as the Ab Roller. To question its utility would have felt only slightly less bizarre than questioning whether humans benefit from going for a little jog. But by the time I aged out of gym class, in the mid-2000s, the sit-up had already begun its quiet disappearance from American fitness. In the years that followed, this iconic exercise would yield its status further. Old-school exercisers may be surprised to hear that this fall from grace is now complete. The sit-up is over. The institutional push to get Americans to exercise started in the 19th century, when federal authorities feared that new kinds of work and mass urban migration were turning a nation of hearty farmworkers into one of sedentary city folk. The situation was regarded as nothing less than a national-security risk—a physically weak nation supplied its military with weak soldiers. These anxieties have long influenced American ideas about fitness, and cemented the link between military exercise practices and civilian exercise trends. So it was that the sit-up, which has been around in one form or another since antiquity, did not fully conquer America until the early 1940s, when the United States Army enshrined it in cadets’ physical training and testing. That decision all but guaranteed that children would be flopping around on the floor at school for the better part of a century afterward. In later years, the U.S. Navy and Marines endorsed the crunch. Whichever variation was in play, military personnel had to complete as many as possible in two minutes—double the time that would later be assigned to grade-schoolers, but otherwise the same test. Our understanding of how the body moves and gains strength has evolved, to put it mildly, in the past 80 years or so. When researchers of old sought to understand the body, they considered its elements separately. “Anatomists would remove the connective tissue around the muscles,” Pete McCall, a personal trainer and fitness educator who has trained instructors for the National Academy of Sports Medicine and the American Council on Exercise, told me. Then they would observe and manipulate the muscles lying flat. That, McCall said, is how they decided that your abdominals pull your spine around, and that your abdominals need to pull your spine around a lot in order to get and stay strong. [Read: What the fitness industry doesn’t understand] Now we know that muscles don’t function alone. Abs are the most visible muscles in a ripped midsection, but they work in concert with a slew of others, including the diaphragm, obliques, erector spinae, and the muscles of the pelvic floor, in order to make all of the tiny movements that most people really only notice after they’ve slept funny. When people talk about the “core,” which has largely replaced “abs” in fitness jargon, they mean all of these muscles, as they work together. But it took decades of research to realize the error, and in the meantime, the decentralized approach to human anatomy became highly influential among another group that has helped to set the conventional wisdom about exercise: Americans trying to get swole. “The first people who popularized all of this exercise were bodybuilders trying to sculpt and define one muscle at a time,” McCall told me. Spot training—the idea that you can effectively remove fat and increase muscle mass in a single area of the body through targeted exercise—is a myth that has been stubbornly resistant to change among novice exercisers, and especially when it comes to abs. The spammy false promise of one weird trick to reduce belly fat lives on in the dregs of internet advertising to this day, precisely because people click on it. As researchers studied more subjects who were upright and, importantly, alive, their understanding of human strength began to change. “If you really want to understand anatomy and how muscles function, you need to understand what they do while the human body is on two feet moving through gravity,” McCall said. When I asked if he could pinpoint the beginning of the end of the sit-up, he directed me to the work of Stuart McGill, a Canadian biomechanics researcher and arguably, he said, the person most responsible for the sit-up’s demise. McGill, a professor emeritus at the University of Waterloo, in Ontario, and the author of the book Back Mechanic, didn’t begin his academic career with a particular interest in the sit-up; his work focused on the spine. But throughout the 1990s and 2000s, he led research that changed the way fitness experts thought about exercise. His findings showed that sit-ups and crunches weren’t just mediocre strength-building moves; they were actually hurting lots of people. “If you bend the spine forward over and over again when not under load, not much happens to the spine,” McGill told me. He gave the example of belly dancers, whose movements he has studied: They flex their spines repetitively without high incidence of injury. “The problem occurs when you flex over and over again with load from higher muscle activation or external objects held in the hands.” If you’ve ever been told to lift with your legs, this is why. When a person’s spine curves and strains in order to move weight through space—like when a bunch of third graders flail through a set of sit-ups—the movement stresses their spinal disks. The more often you ask your spine to flex in those circumstances, the riskier it is. This is how people who spend their working lives moving inventory around a warehouse or stacking bushels of produce onto trucks end up with back pain later in life, even if they can’t point to any acute back injuries suffered along the way. McGill found that the most reliable way to avoid this kind of chronic problem is to brace your core when you pick up something heavy. That means tensing key muscles in order to protect your spine’s structural integrity, and to help shift the effort to your hips and legs. Not coincidentally, weight lifters follow this advice when they safely execute a dead lift. Perfect form is not always possible for workers dealing with irregular loads and crowded spaces, but intentional exercise is all about form. Getting it right and activating the intended muscles is the whole point. The sit-up and crunch violate all of these principles. The exercise asks you to pick up something heavy, but because you’re lying on the ground and the heavy thing is your upper body, there’s no way for you to brace your core and shift the effort to the big, high-capacity muscles of your legs. And the exercise is, by its nature, repetitive. For generations, schoolchildren and troops were both told to do as many sit-ups or crunches as possible in order to score well on compulsory testing. Some people can do these exercises with no problem, McGill stipulated, but that capability depends largely on genetic factors such as how light- or heavy-framed a person is, not on any particular executional skill. For population-level instruction and testing, the sit-up simply does not work. As McGill and other experts published their findings, he began to hear from people who had found injury patterns that matched his research—most notably, from trainers and physical therapists in the U.S. and Canadian military, who were questioning the sit-up’s primacy in their fitness instruction. In the past decade, every branch of the U.S. military has begun to phase out sit-ups and crunches from their required testing and training regimens, or else they have made them optional, alongside more orthopedically sound maneuvers such as the plank. Spokespeople for the Army and the Marines confirmed to me that these decisions in their branches were made in part to avoid the high rates of lower-back injury found among troops training for speed sit-up and crunch tests. According to McCall, the fitness educator, when the military decides that a long-standard exercise is no longer up to snuff, lots of trainers take notice. Because of the scale and prestige of the military’s training programs, their institutional practices remain highly influential on civilian exercise, which has helped to hustle the sit-up further to the margins over the past few years. Childhood fitness testing has relented, too. The Presidential Youth Fitness Program, which replaced the Presidential Fitness Test almost a decade ago, now recommends that children practice curl-ups, which are a much more subtle movement developed by McGill that asks exercisers to brace their core while lifting their head and shoulders only slightly. (If your fitness routine regularly includes planks, bird dogs, or dead bugs, that’s also McGill’s doing—he didn’t develop those exercises, but he did usher them into mainstream use as sit-up alternatives.) If you hadn’t yet noticed crunches disappearing around you—or if you have a trainer who still puts you through your sit-up paces—McCall said he wouldn’t exactly be shocked. Like many other American industries, the fitness business is consolidating, but it still contains tons of independent instructors and small businesses. Sit-ups and crunches have been discouraged by educators within the industry for years, but there are no licensing or continuing-education requirements for teaching exercise, and if trainers don’t seek out new information and techniques, it can take a while for good information and new ideas to get through to them. Even up-to-date instructors may have plenty of clients who just won’t let go of exercise as they’ve always understood it. “A good trainer will educate the client,” McCall told me. “But the sad fact is, with some clients, if you didn’t have them do two or three sets of crunches, they would feel like they’re not getting a good workout.” from https://ift.tt/7iCIy9h Check out http://natthash.tumblr.com
0 Comments
Two and a half years and billions of estimated infections into this pandemic, SARS-CoV-2’s visit has clearly turned into a permanent stay. Experts knew from early on that, for almost everyone, infection with this coronavirus would be inevitable. As James Hamblin memorably put it back in February 2020, “You’re Likely to Get the Coronavirus.” By this point, in fact, most Americans have. But now, as wave after wave continues to pummel the globe, a grimmer reality is playing out. You’re not just likely to get the coronavirus. You’re likely to get it again and again and again. “I personally know several individuals who have had COVID in almost every wave,” says Salim Abdool Karim, a clinical infectious-diseases epidemiologist and the director of the Center for the AIDS Program of Research in South Africa, which has experienced five meticulously tracked surges, and where just one-third of the population is vaccinated. Experts doubt that clip of reinfection—several times a year—will continue over the long term, given the continued ratcheting up of immunity and potential slowdown of variant emergence. But a more sluggish rate would still lead to lots of comeback cases. Aubree Gordon, an epidemiologist at the University of Michigan, told me that her best guess for the future has the virus infiltrating each of us, on average, every three years or so. “Barring some intervention that really changes the landscape,” she said, “we will all get SARS-CoV-2 multiple times in our life.” If Gordon is right about this thrice(ish)-per-decade pace, that would be on par with what we experience with flu viruses, which scientists estimate hit us about every two to five years, less often in adulthood. It also matches up well with the documented cadence of the four other coronaviruses that seasonally trouble humans, and cause common colds. If SARS-CoV-2 joins this mix of microbes that irk us on an intermittent schedule, we might not have to worry much. The fact that colds, flus, and stomach bugs routinely reinfect hasn’t shredded the social fabric. “For large portions of the population, this is an inconvenience,” Paul Thomas, an immunologist at St. Jude Children’s Research Hospital, in Tennessee, told me. Perhaps, as several experts have posited since the pandemic’s early days, SARS-CoV-2 will just become the fifth cold-causing coronavirus. Or maybe not. This virus seems capable of tangling into just about every tissue in the body, affecting organs such as the heart, brain, liver, kidneys, and gut; it has already claimed the lives of millions, while saddling countless others with symptoms that can linger for months or years. Experts think the typical SARS-CoV-2 infection is likely to get less dangerous, as population immunity builds and broadens. But considering our current baseline, “less dangerous” could still be terrible—and it’s not clear exactly where we’re headed. When it comes to reinfection, we “just don’t know enough,” says Emily Landon, an infectious-disease physician at the University of Chicago. [Read: Coronavirus reinfection will soon become our reality] For now, every infection, and every subsequent reinfection, remains a toss of the dice. “Really, it’s a gamble,” says Ziyad Al-Aly, a clinical epidemiologist and long-COVID researcher at Washington University in St. Louis. Vaccination and infection-induced immunity may load the dice against landing on severe disease, but that danger will never go away completely, and scientists don’t yet know what happens to people who contract “mild” COVID over and over again. Bouts of illness may well be tempered over time, but multiple exposures could still re-up some of the same risks as before—or even synergize to exact a cumulative toll. “Will reinfection be really bad, or not a big deal? I think you could fall down on either side,” says Vineet Menachery, a coronavirologist at the University of Texas Medical Branch. “There’s still a lot of gray.” The majority of infections we witnessed in the pandemic’s early chapters were, of course, first ones. The virus was hitting a brand-new species, which had few defenses to block it. But people have been racking up vaccine doses and infections for years now; immunity is growing on a population scale. Most of us are “no longer starting from scratch,” says Talia Swartz, an infectious-disease physician, virologist, and immunologist at Mount Sinai’s Icahn School of Medicine. Bodies, wised up to the virus’s quirks, can now react more quickly, clobbering it with sharper and speedier strikes. Future versions of SARS-CoV-2 could continue to shape-shift out of existing antibodies’ reach, as coronaviruses often do. But the body is flush with other fighters that are much tougher to bamboozle—among them, B cells and T cells that can quash a growing infection before it spirals out of control. Those protections tend to build iteratively, as people see pathogens or vaccines more often. People vaccinated three times over, for instance, seem especially well equipped to duke it out with all sorts of SARS-CoV-2 variants, including Omicron and its offshoots. Gordon, who is tracking large groups of people to study the risk of reinfection, is already starting to document promising patterns: Second infections and post-vaccination infections “are significantly less severe,” she told me, sometimes to the point where people don’t notice them at all. A third or fourth bout might be more muted still; the burden of individual diseases may be headed toward an asymptote of mildness that holds for many years. Gordon and Swartz are both hopeful that the slow accumulation of immunity will also slash people’s chances of developing long COVID. An initial round of vaccine doses seems to at least modestly trim the likelihood of coming down with the condition, and the risk may dwindle further as defenses continue to amass. (“We do need more data on that,” Gordon said.) [Read: The pandemic after the pandemic] Immunity, though, is neither binary nor permanent. Even if SARS-CoV-2’s assaults are blunted over time, there are no guarantees about the degree to which that happens, or how long it lasts. Maybe most future tussles with COVID will feel like nothing more than a shrimpy common cold. Or maybe they’ll end up like brutal flus. Wherever the average COVID case of the future lands, no two people’s experience of reinfection will be the same. Some may end up never getting sick again, at least not noticeably; others might find themselves falling ill much more frequently. A slew of factors could end up weighting the dice toward severe disease—among them, a person’s genetics, age, underlying medical conditions, health-care access, and frequency or magnitude of exposure to the virus. COVID redux could pose an especially big threat to people who are immunocompromised. And for everyone else, no amount of viral dampening can totally eliminate the chance, however small it may be, of getting very sick. Long COVID, too, might remain a possibility with every discrete bout of illness. Or maybe the effects of a slow-but-steady trickle of minor, fast-resolving infections would sum together, and bring about the condition. Every time the body’s defenses are engaged, it “takes a lot of energy, and causes tissue damage,” Thomas told me. Should that become a near-constant barrage, “that’s probably not great for you.” But Swartz said she worries far more about that happening with viruses that chronically infect people, such as HIV. Bodies are resilient, especially when they’re offered time to rest, and she doubts that reinfection with a typically ephemeral virus such as SARS-CoV-2 would cause mounting damage. “The cumulative effect is more likely to be protective than detrimental,” she said, because of the immunity that’s laid down each time. Al-Aly sees cause for worry either way. He is now running studies to track the long-term consequences of repeat encounters with the virus, and although the data are still emerging, he thinks that people who have caught the virus twice or thrice may be more likely to become long-haulers than those who have had it just once. There’s still a lot about SARS-CoV-2, and the body’s response to it, that researchers don’t fully understand. Some other microbes, when they reinvade us, can fire up the immune system in unhelpful ways, driving bad bouts of inflammation that burn through the body, or duping certain defensive molecules into aiding, rather than blocking, the virus’s siege. Researchers don’t think SARS-CoV-2 will do the same. But this pathogen is “much more formidable than even someone working on coronaviruses would have expected,” Menachery told me. It could still reveal some new, insidious qualities down the line. Studying reinfection isn’t easy: To home in on the phenomenon and its consequences, scientists have to monitor large groups of people over long periods of time, trying to catch as many viral invasions as possible, including asymptomatic ones that might not be picked up without very frequent testing. Seasonal encounters with pathogens other than SARS-CoV-2 don’t often worry us—but perhaps that’s because we’re still working to understand their toll. “Have we been underestimating long-term consequences from other repeat infections?” Thomas said. “The answer is probably almost certainly yes.” Of the experts I spoke with for this story, several told me they hadn’t yet been knowingly infected by SARS-CoV-2; of those who had, none were eager for the sequel. Menachery is in the latter group. He was one of the first people in his community to catch the virus, back in March of 2020, when his entire family fell ill. That November, he discovered that he had lost most of his kidney function, a rapid deterioration that he and his doctors suspect, but cannot prove, was exacerbated by COVID. Menachery received a transplant three months ago, and has been taking immunosuppressive medications since—a major shift to his risk status, and his outlook on reinfection writ large. “So I wear my mask everywhere,” he told me, as do his wife and their three young kids. Should the virus return for him, it’s not totally clear what might happen next. “I’m nervous about reinfection,” he said. “I have reason to be.” Almost no one can expect to avoid the virus altogether, but that doesn’t mean we can’t limit our exposures. It’s true that the body’s bulwarks against infection tend to erode rather rapidly; it’s true that this virus is very good at splintering into variants and subvariants that can hop over many of the antibodies we make. But the rhythm of reinfection isn’t just about the durability of immunity or the pace of viral evolution. It’s also about our actions and policies, and whether they allow the pathogen to transmit and evolve. Strategies to avoid infection—to make it as infrequent as possible, for as many people as possible—remain options, in the form of vaccination, masking, ventilation, paid sick leave, and more. “There are still very good reasons” to keep exposures few and far between, Landon, of the University of Chicago, told me. Putting off reinfection creates fewer opportunities for harm: The dice are less likely to land on severe disease (or chronic illness) when they’re rolled less often overall. It also buys us time to enhance our understanding of the virus, and improve our tools to fight it. “The more we know about COVID when we get COVID,” the better off we’ll be, she said. [Read: The coronavirus’s next move] SARS-CoV-2 may yet become another common-cold coronavirus, no more likely to screw with its hosts the fifth time it infects them than the first. But that’s no guarantee. The outlooks of the experts I spoke with spanned the range from optimism to pessimism, though all agreed that uncertainty loomed. Until we know more, none seemed too eager to gamble with the virus—or with their own health. Any reinfection will likely still pose a threat, “even if it’s not the worst-case scenario,” Abdool Karim told me. “I wouldn’t want to put myself in that position.” from https://ift.tt/GI42wWP Check out http://natthash.tumblr.com The first data on Paxlovid, out last November, hinted that the COVID antiviral would cut the risk of hospitalization and death by 89 percent. Pundits called the drug “a monster breakthrough,” “miraculous,” and “the biggest advance in the pandemic since the vaccines.” “Today’s news is a real game-changer,” said Albert Bourla, the CEO of Pfizer, which makes the drug. The pills are “a game changer,” President Joe Biden repeated a few months later. Now, finally, the game is being changed. The government has ordered 20 million courses of Paxlovid, committing half of the $10 billion in additional COVID funding that is being negotiated in the Senate; and Pfizer says that the number of patients taking the drug increased by a factor of 10 between mid-February and late April. But as the treatment spreads, so too does confusion over its effectiveness and side effects. Patients have complained of a bitter, metallic taste, or one like grapefruit juice mixed with soap, the whole time they were on the drug. More concerning, some have reported experiencing a second round of symptoms, and going back to testing positive, when the pills were done, a phenomenon that’s become known as “Paxlovid rebound.” Meanwhile, Pfizer has never published any final data on the use of the drug by vaccinated patients, leaving medical professionals with little information about how the drug works for people who have received their shots—which is to say, most of the adult population in the U.S. “We’re all riding on hope at this point,” Reshma Ramachandran, a family-medicine doctor at Yale, told me. [Read: Paxlovid mouth is real—and gross] An individual patient would never know if Paxlovid worked for them, because you could never say how sick you would have gotten if you hadn’t taken the pills. If the drug doesn’t really do that much for vaccinated people—if it fails to have meaningful effects on their risk of severe disease, and doesn’t help resolve their symptoms—then giving it out widely could be a waste of the dwindling resources the United States has committed to fight the pandemic, not to mention physicians’ time and patients’ sense of taste. And because people who have just recovered from COVID might reasonably believe they’re in the clear, and mingle with abandon, surprise cases of Paxlovid rebound could end up causing more transmission. “We continue to monitor data from our ongoing clinical studies and post-authorization safety surveillance,” a Pfizer spokesperson told me in an email, noting that cases of viral rebound “are being reported at a rate consistent with observations” from the company’s published clinical trial. Taste disruption (a.k.a. dysgeusia) is the most straightforward of the Paxlovid mysteries, because any sudden onset of soapy-grapefruit-penny flavor can be attributed to the antiviral with a decent amount of confidence. In its only published trial of the drug, conducted in unvaccinated, high-risk patients, Pfizer found that 5.6 percent of Paxlovid-takers experienced dysgeusia, compared with 0.3 percent of those who got the placebo. If you apply that rate to the hundreds of thousands of people who have now received the drug, you might expect to see some tens of thousands of cases by now. Given how people like to kvetch on social media, that side effect could very well seem like it’s occurring in a lot more than one out of 18 patients. Perhaps all that’s going on here is that rare events seem common on a large scale. Perhaps! But I’ve heard from dozens of patients on the drug in the course of my reporting, and every single one told me that they’d suffered through at least mild dysgeusia. Paul Sax, the clinical director of the Division of Infectious Diseases at Brigham and Women’s Hospital, told me he suspects “way more than half” of the people who’ve taken Paxlovid have experienced the taste. As for rebound, a Pfizer executive said during an earnings call this month that the company had taken a “preliminary look” at its trial data and concluded that viral loads bounced back up in about 2 percent of patients. He also said they saw “the same or close to the same percent in the placebo arm.” (These findings have not been published.) “Reports from the beginning of the pandemic suggested some participants exhibit fluctuations in nasal viral RNA, and these fluctuations could be a phenomena [sic] of the disease itself,” the Pfizer spokesperson told me. In any case, if you apply that measured rate of 2 percent to the population who have now taken the drug, you’d expect thousands of people to have experienced Paxlovid rebound by this point (and many, many more cases of rebound occurring among all the COVID patients who didn’t take it). The real number is—well, we have pretty much no idea what the real number is. The federal government is not tracking Paxlovid rebound in any public-facing database, and the CDC released an advisory on Tuesday saying the agency doesn’t know whether a recurrence of symptoms can be connected to the drug. The agency also clarified that “Paxlovid continues to be recommended for early stage treatment of mild to moderate COVID-19 among persons at high risk for progression to severe disease” and that anyone who rebounds should isolate for another five days. No researchers have yet published studies measuring the prevalence of rebound, but a good number of clinicians and Paxlovid patients are convinced that it’s higher than 2 percent. “To trust that number would’ve been to not believe my eyes,” Bob Wachter, the chair of medicine at UC San Francisco, told me. In an attempt to find some clarity, Wachter decided to poll his Twitter connections on whether they’d taken Paxlovid and rebounded. (I’m legally obligated to tell you that Twitter polls are neither scientific nor particularly reliable—which Wachter knows perfectly well.) Of the respondents who said they had taken Paxlovid, 45 percent rebounded; Wachter said he guesses the real proportion is closer to 10 or 20 percent. A few hours after we spoke, Wachter tweeted that his wife, who had recently finished a course of the antiviral and recovered from COVID, just tested positive again. In short, Pfizer’s clinical-trial results may not be matching up with physicians’ and patients’ real-world experience. When I asked the company why, the spokesperson replied, “We cannot speculate on why some people may or may not experience dysgeusia, but we can reiterate that 5.6% of participants in a well-controlled clinical trial experienced that event compared to 0.3% in the placebo arm.” As for rebound, he said, the company continues to monitor the data but hasn’t yet seen any unexpected numbers. “We are actively reviewing but, thus far, have not seen an association with subsequent severe disease (i.e., hospitalization or death),” he added. Discrepancies between the trial data and real-world experience might arise from the timing of the original research. Pfizer announced its results in early November, which means that participants received Paxlovid to help fight off infections caused by the Delta variant, which is naught but an unpleasant memory today. Three Omicron subvariants are currently floating through Americans’ airways. Perhaps one of them simply causes more rebound cases than Delta did, by keeping viral levels high enough that five days of antiviral therapy are not enough to wipe it out. Anthony Fauci announced last week that the National Institutes of Health is in talks with Pfizer to test out a longer course of Paxlovid to see if it reduces rates of rebound. (“We will share updates when we have them,” the Pfizer spokesperson said.) In the meantime, Bourla, Pfizer’s CEO, has suggested that those who experience a rebound should simply take another round of Paxlovid. But the FDA was less than enthusiastic about the idea. Patients’ immunization status remains the most obvious difference between Pfizer’s published clinical trial and present-day reality. That study was conducted exclusively in unvaccinated participants who were at high risk of complications from COVID. The drug is now authorized for use in vaxxed and unvaxxed patients alike. Could this explain the apparent gulf in the prevalence of bad tastes and rebound? Ali Ellebedy, an immunologist at Washington University in St. Louis, told me he couldn’t imagine any direct link between vaccination and Paxlovid rebound or dysgeusia. And if anything, he said, immunological principles suggest that, compared with unvaccinated people, the vaccinated should have fewer cases of rebound, not more. Then again, “with COVID over the last two and a half years, we have been wrong--I have been wrong—so many times,” he said. Providers are certainly anxious to know how many of their vaccinated patients experience Paxlovid rebound. But on a more basic level, they’re anxious to know how well the drug works in vaccinated people at all. “We really know nothing about the magnitude of its benefit or its risk in people who are vaccinated, let alone triple or quadruple vaccinated,” Walid Gellad, who directs the University of Pittsburgh’s Center for Pharmaceutical Policy and Prescribing, told me. Without that information, if a doctor has to decide whether to prescribe Paxlovid to a patient who’s eligible, “you make your best guess,” Gellad said. Pfizer has hinted at some sunny results in vaccinated people, but no data have been made publicly available. Also, way back in December, the company said it had finished enrolling participants for a follow-up study of Paxlovid in people who are not at high risk of severe COVID. But then, a few months later, it changed the eligibility criteria to leave out anyone who had received a vaccine dose in the preceding 12 months.. Today, that follow-up trial is still listed as in the “recruiting” phase on ClinicalTrials.gov. Reshma Ramachandran said the changes are a “red flag” that Pfizer might have uncovered some preliminary results among vaccinated participants that weren’t so flattering. David Boulware, a clinical-trial expert at the University of Minnesota, told me that he thinks the rationale for Pfizer’s actions is “pretty obvious”: The company will have an easier time proving the drug works in people who are more likely to be hospitalized—that is, the unvaccinated (and those whose vaccinations are more than a year old). “From a pure researcher perspective, I can understand exactly why they did this. But from a public-health and just, like, being-a-physician perspective, it’s a terrible idea.” The Pfizer spokesperson told me that the company had limited enrollment to patients who had not received a vaccine dose for at least a year in order to “enrich the study population for individuals whose immunity may be waning and who may be at elevated risk of severe COVID-19, hospitalization or death.” To make the best decisions possible regarding prescribing Paxlovid, doctors and patients would need to understand how common rebounds are, whether the drug causes them, and whether people are infectious during the rebound period. They’d also need to know whether the drug has any meaningful benefits for people who have gotten a primary vaccine dose or booster shot since May 2021. Boulware said he expects researchers in the United Kingdom to have data on Paxlovid’s efficacy in vaccinated people within the next couple of months. Gellad is also eager to know whether Paxlovid helps stave off long COVID, a hypothesis that would by definition take months or years to test. Ali Ellebedy is curious about whether taking Paxlovid dulls a patient’s immune response to the virus and therefore could leave them more vulnerable the next time they encounter it. Until those questions are answered, the providers I spoke with are all erring on the side of prescribing Paxlovid. “You’re kind of stuck as a prescriber,” Gellad said. Doctors could wait and advise their vaccinated patients not to take the drug until they’re certain it’ll help, but vaccinated people are still getting sick, developing long COVID, going to the hospital, and dying. To draw a balance between caution and action, Ramachandran said that when she prescribes Paxlovid to her vaccinated patients, she also explains that the clinical trials weren’t conducted in people like them, and so exactly what they’ll get out of the drug is uncertain. “When we’re trying to look for options for COVID-19, especially for treatment, we just have so few options,” she said. For now, Paxlovid is the best bet. from https://ift.tt/WUP5KSg Check out http://natthash.tumblr.com Nearly 15 years ago, a young man who had shot himself in the head with his father’s gun was wheeled into the emergency room where Megan Ranney worked. Despite her team’s best efforts, the patient died. “It was the first firearm suicide I’d ever taken care of,” Ranney, an emergency physician and public-health expert in Rhode Island, told me. In the days after, Ranney found herself wondering about the circumstances that had landed that boy in her hospital. What had made that gun so easily accessible? Why had he reached for it? What had failed to stay his hand? In the decade-plus since, many, many more firearm injuries have crossed her path—“truly, I can’t even count the number of folks I’ve taken care of who have been shot,” she said. Each year, guns kill tens of thousands of people in the United States; on Tuesday, an 18-year-old gunman added at least 21 more to 2022’s horrific tally, when he entered an elementary school in Uvalde, Texas, and opened fire in a fourth-grade classroom. Like other mass shootings, this one has turned the national conversation toward laws that could cut down on firearm-related deaths (of which mass shootings make up just a small fraction). And it’s true: Policy change could make a difference. But if history tells us anything, chasing after legislation will not reduce gun deaths on its own. Firearm injuries, Ranney said, are also a public-health crisis that demands public-health solutions—ones that can be enacted not just by the nation’s leaders in the future, but by individuals and communities right now. America has, of course, been squaring off with a very different sort of epidemic over the past two and a half years. COVID has showcased the power of public-health initiatives. It has also forced us to acknowledge what happens when those same efforts falter. Outbreaks of infectious disease are complex: They are about pathogens, yes, but also the people who ferry them from place to place, the tools we use to hamper their spread, and the preventive behaviors communities are and are not willing to take. They spread fast and disproportionately affect certain people, but they can be stopped before they spiral out of control. In much the same way, “there is a long pathway that gets people to the point where they pick up a gun with the intention to hurt themselves or another,” said Ranney, who five years ago co-founded AFFIRM at the Aspen Institute, an initiative taking a health-based approach to ending the American firearm-injury epidemic. I called Ranney to talk to her about the public-health approach to reducing firearm injury. Our conversation has been edited for clarity and length. Katherine J. Wu: Explain why firearm injury is a public-health problem, and not just a policy one. Megan Ranney: People continue to harden into these two extreme positions: Get rid of all guns, or give everybody a gun. Gun rights versus gun control. When there’s a shooting, the two sides get louder and louder, and further and further apart. The way that we have been approaching this is clearly not working. But there is a third way, which is addressing this as a health problem, which this very much is. It brings people into my ER day after day. Core to public health is the idea that you have to think on a larger scale—not just about the patient in front of you, but also about individual- and population-level risk factors, and how to modify and reduce them. Some of that might be about the firearm and policy related, but some are also going to be about the person, and some are going to be about the neighborhood or the structure. We talk about car crashes as a health problem. We’ve set up whole systems to reduce car-crash injury and death. We talk about heart attacks as a health problem, and we’ve set up whole systems to reduce the incidence and severity of heart attacks. Why are we not doing the same thing for guns? And I want to be specific that I’m talking about firearm injury, not about the firearms themselves. For motor-vehicle crashes, the car is that mechanism, but our goal is to reduce the crash, and the death on the other side. Wu: What does a public-health approach offer us? Is there another instance in which policy solutions have faltered, or become stagnant, and public health was able to successfully step in? Ranney: Car crashes are the example that I most frequently bring up. By some metrics, we’ve decreased the number of car crash deaths by about 70 percent since the 1970s—not by banning cars, but rather by making cars safer, by making drivers safer, and by developing car seats and teaching parents how to use them. There’s a combination of education, engineering, and policy that has been put in place to decrease car-crash deaths. Another example is HIV. We’ve used science and the public-health approach to identify what causes HIV and help reduce its transmission, as well as its likelihood of causing death. Yes, it’s about basic research and antiretrovirals. But it’s also about a harm-reduction approach around safer sex, safe syringe-needle use, safe injection sites, and giving people the tools to advocate for themselves. These two examples both illustrate this core belief in public health, which is that you can identify risk factors and then empower individuals, as well as change society. Part of the public-health approach is also saying that we’re not going to get to zero. If we could go back to the number of gun injuries and deaths that we had ten years ago? We’d be looking at 40 percent fewer than we have today. But it requires moving beyond this all-or-nothing approach. Wu: And yet, gun violence is so often framed in the arena of policy—of which laws are and are not being passed. Why isn’t that enough on its own? Ranney: Policies are so important in public health. But they are only as effective as the community norms in which those policies are passed. An example: Safe storage is one of the most important things that we can do to reduce risk of firearm suicide and homicide. Most youths who kill themselves with a gun use a family member’s gun. Most youths who commit a school shooting use a family member’s gun. Safe storage—making sure that your gun is locked up and not accessible to your kid—is a major way to prevent that. Safe storage is also important in terms of reducing the flow of illegal guns on the streets, which causes firearm homicide. We’ve seen a skyrocketing number of guns being stolen from cars because they’re not being stored safely in those cars. In order to get folks to store guns safely, policies can make a difference. But more important is the firearm-owning community standing up for how important safe storage is—making this part of the purchase of a gun, part of the community norm around firearm ownership, and part of a discussion between friends or family members. And that second part is the public-health approach. It’s about not putting all of our eggs in the basket of policy, but instead thinking also about the structural drivers. And it’s about involving the very communities that most need to be at the table in order to reduce the risk of injury and death, which is gun owners. Wu: So what are some actionable steps that can be taken, within this public-health framework? Ranney: One of the biggest things that we can invest in is data. For more than 20 years, there was pretty much no federal funding for firearm-injury-prevention research. As a result, the evidence behind how to stop firearm injuries before they happen stalled. We’re basically in the same place that we were in the 1990s. Imagine if that were true for heart disease or for HIV. That would be unacceptable. In the last few years, we’ve finally restarted firearm-injury-prevention research. There’s no way that we’re going to make sustained, real change without investing in collecting the data. That’s not going to change the numbers of kids who are in danger tomorrow, but it’s an essential part of bending the curve on this disease for the long term. The other structural solution is again to stand up for the fact that public health matters. Making sure that your local public-health department is budgeted for adequately and that community organizations are supported makes a difference. It’s about getting both sides of the table and creating partnerships between firearm owners and non–firearm owners that can help to identify those at risk and reduce the risk. Wu: What changes can begin immediately at the individual and community levels? Ranney: The first thing is to allow yourself time to grieve. You can also talk to your kids, both to help them process what has happened and to be a safe space for them if they notice something concerning about a friend, either on social media or in school. The second thing is that if you yourself are a firearm owner, or if you have a family or are in a neighborhood where firearms are common, you can have discussions about safe storage, about how to identify risk factors, and about how to help the start to change cultural norms around what safe, responsible firearm ownership looks like and how to reduce the risk of gun misuse. The third thing that you can do today is to get involved in community organizations that help to create those spaces that look out for each other. One of the biggest predictors of violence is being isolated. The way that we address that is by getting together long before the shooting happens. Some of the best ways to reduce violence are around things like Boys & Girls Clubs, or putting in place community gardens. A great example is the work that a colleague of mine, Eugenia South, is doing in Philadelphia, around greening vacant lots. When you put in a community garden, you not only decrease the number of firearms injuries in that neighborhood, but you also decrease stress, depression, and other problems as well. It’s a very discrete and doable intervention that can help shift the patterns for our community. Yes, policy change matters and letting your congresspeople know that certain policies make a big difference. But there are things you can do, long before you get there. Wu: We’ve seen what public-health approaches can do these past two years, and also what happens when we don’t take it seriously. Has COVID shifted your approach to gun violence? Ranney: There are a few lessons that stick out. One is the importance of community involvement, clear communication, and trusted messengers from the get-go. We developed amazing vaccines, but we never did the work to make sure that folks trusted them, to make sure that they were accessible, and to make sure that we were prepared to combat not only disinformation but also an absence of information that continues to plague many communities across the United States. And the same thing can be applied to firearm injury. We cannot fix this problem if we don’t pay attention to the communities and the people living in those communities in which gun deaths happen—if we don’t have their voices elevated and have them out there talking about why and how to prevent gun deaths. Another is around harm reduction: allowing people to live their lives in a way that reduces the risk of infection and death, in the context of COVID. How do we reduce deaths instead of trying to get them to zero? We saw this all-or-nothing attitude during COVID, and it really hurt our ability in the U.S. to get COVID under control. The same is true for firearms. Anyone who thinks that we are going to get rid of firearms in this country is not living in the United States that I live in. Some absolutist nirvana is never going to happen. Instead, everyone needs to work with communities to create solutions that creep forward progress. I’ve seen really clear examples of how you can make progress on these seemingly divisive issues. It takes time and hard work, but it is possible. And what choice do we have? It’s so easy to just dismiss this as another tragedy that you kind of feel hopeless about, and go on with your day. Knowing that there are both big-picture things that you can do, but also small-picture things that you can do, is essential. These kids and all the people who die every day deserve better than for us to forget them. from https://ift.tt/RxijNoX Check out http://natthash.tumblr.com For the past year and a half, since the COVID-19 vaccines first became available—even as last summer’s reprieve gave way to Delta’s surge, then Omicron’s; even as the coronavirus continued to rack up mutations that lifted its speed and its stealth; even as millions of vaccinated Americans caught the pathogen and passed it on—there’s been one huge slice of solace to cling to: The shots we have are still doing an excellent job of staving off severe disease and death. Billions of people around the world have now been dosed at least once, twice, or thrice; the shots have saved an estimated hundreds of thousands of lives—and they probably could have saved hundreds of thousands more in the United States alone, had more people rolled up their sleeves. “We’re so much better off than where we were in 2020, when nobody had any immunity,” says Donna Farber, an immunologist at Columbia University. It feels, in some ways, like gazing down the side of a mountain we’ve been trekking up for a good 30 months: A nice, stubborn buffer of elevation now lies between us and the bottom, the sea-level status of no protection at all. The body’s defenses against severe disease are immunological bedrock—once cemented, they’re quite difficult to erode. Even as the fast-mutating virus pushes down from above, our footing has, for more than a year now, felt solid, and the ground beneath us unlikely to give. [Read: America is starting to see what COVID immunity really looks like] The shots aren’t perfect: They can’t completely block infections or keep the debilitating symptoms of long COVID at bay. Still, against the severest outcomes, “I think vaccination is holding up,” Ali Ellebedy, an immunologist at Washington University in St. Louis, told me. “It provides a lot of comfort, just knowing that layer is there,” says Natalie Dean, a biostatistician at Emory University. As SARS-CoV-2’s shape-shifting shenanigans continue, though, widening the evolutionary chasm between its current iteration and the version that inspired 2020’s vaccines, our position is starting to feel more precarious. Say our immune defenses weaken, and cause us to slip; say the virus ups the ante again, and delivers a particularly powerful blow. A rapid tumble down to the trailhead—a total immunological reset—still seems very, very unlikely. The further away we stay from that juncture, though, the better off we’ll be. If minimizing severe disease is a summit of sorts, it’s one we have to keep striving for, likely by revaccinating, and hopefully with updated shots. Knowing when to dose up again, and with what, will require keeping close watch on local conditions, trying to anticipate how the virus might shove us, and maintaining our gear in tip-top shape. It’s a long way to the bottom, but backslides are possible. Stopping severe disease and death is the first goal of any vaccine. But it’s not necessarily the first protective pinnacle the world set its sights on. Back when the vaccines were new and a near-perfect match for the circulating strain, many people felt hopeful that we’d quickly clamber up to some Symptom-Free Vista—maybe even dart up to No-Infection Point. As the vaccines got further out from their debut, however, it became clear that we weren’t going to be camping at those outcrops long-term. Which is pretty expected: For any immunization to sustainably and reliably keep people safe from all infections is rare. In the months after people get their shots, levels of infection-blocking antibodies naturally drop off, making it easier for pathogens to infiltrate the body and reproduce. At the same time, the virus is only getting better at knocking us down—it strikes a new blow each time it tacks on another mutation that distances it from the version of itself that inspired our shots. That wild card worries experts far more than any immunological stumble. “Virus evolution is always my biggest concern,” Ellebedy told me. Members of the Omicron clan—the most formidable branch of the SARS-CoV-2 family to date—have proved themselves deft at infecting even the multiply vaccinated, slipping around shot-raised antibodies with ease. Immunity is too multifaceted, too broad, and too flexible for SARS-CoV-2 to shove us all the way down to the mountain’s base; although speedy defenders such as antibodies decline in the short term, other soldiers such as B cells and T cells can stick around for years, even decades, stowing intel on the virus so they can rise up again. These veteran fighters aren’t fast enough to stop a virus from breaching the body’s barriers. But when it does, they can trounce it before the infection gets too severe. They’re also far harder to stump than fickle, fragile antibodies; even weird morphs like Omicron are familiar-looking enough to evoke the ire of most vaccine-trained T cells and an appreciably large fraction of B cells. “That protects us, even if antibodies are lost,” says Hana El-Sahly, an infectious-disease physician at Baylor College of Medicine. Still, the virus’s assaults on our position on the flanks of Protection Peak are getting stronger. We’ve had to dig our heels in far deeper to stay the course. Two doses of mRNA vaccine, for instance, were enough to hold the line against SARS-CoV-2 in the Delta era and before. Omicron’s mutations, though, upped the ante and made the mountain more formidable. The latest estimates provided by the CDC, which run through the first part of winter, suggest that adults who have received a duo of mRNA doses can cut their risk of serious sickness from Delta by at least 80 to 95 percent; the numbers drop into the 50ish to 70ish range with the original iteration of Omicron, or BA.1, subbed in. So experts recommended an equipment upgrade to keep the summit in sight: another dose, which can restore the body’s ability to stave off severe disease from BA.1 at rates of about 75 to 90 percent. What’s not certain, though, is how long SARS-CoV-2 will continue to rest on its laurels. Faced with growing population immunity, the virus is being forced to repeatedly switch up its appearance. In the span of just a few months, Omicron has already sprouted several new alphanumeric offshoots—BA.2.12.1, BA.4, and BA.5—that can dodge the defenses that even a tussle with their sibling BA.1 leaves behind. And it’s not entirely clear how wild SARS-CoV-2’s costume changes could get. Parts of the virus that scientists once thought were unlikely to change much have since transformed. This coronavirus, like others that have come before it, has shown a remarkable capacity to shape-shift when faced with immunity blockades, says David Martinez, a viral immunologist at the University of North Carolina at Chapel Hill. “There’s a lot of real estate left in spike,” he told me, “for the virus to continually evolve.” Our vaccines, meanwhile, remain modeled on a version of the virus that first infiltrated the population more than two years ago, and that has since disappeared. “Yes, vaccine effectiveness remains really high” against severe disease, even months out, even against Omicron, says Saad Omer, an epidemiologist at Yale University. But that doesn’t mean there isn’t room to relace our boots and attempt to ascend again. Just how well protected we are right now—how close to the bottom or the top of the peak—isn’t totally clear. “Our ability to capture this is clouded,” Dean told me. So much of the landscape we’ve been meandering upon has shifted in recent months; we, the travelers, have also changed. To really get a good grip on vaccine performance, Dean said, researchers need to carefully track large groups of people who have gotten different numbers of shots—anywhere from zero to three or more—over long periods of time, carefully tabulating who’s getting infected, sick, hospitalized, or killed. Metrics like these were relatively easy to monitor during the shots’ clinical trials. But the real world is far messier, and gathering data is much more difficult now. That’s especially true in the U.S., which lacks a nationalized health-care system, and has no single, uniform way to record-keep. Americans’ immunization options also keep splintering. Shots are being administered to different people at different intervals, in different combinations, against different variants; successes and failures against the virus are now much harder to tie directly to the potency of the injections themselves. Vaccinated and unvaccinated people have also gotten way more challenging to compare: They belong to very different demographic groups, split apart by when (or if) they became eligible and how vulnerable to the virus they are, as well as the allegiances that might have swayed some of them toward opting into or out of shots. It’s also getting rougher and rougher to statistically account for how the pandemic, and the response to it, has evolved. Vaccines work better against all outcomes when the bodies they’re protecting aren’t constantly being taxed by heavy, frequent exposures to a pathogen; in recent months, mask mandates have lifted, and crowded indoor gatherings have gone back into full swing. On the flip side, treatments such as Paxlovid have become more available, muddying patterns that could help clue researchers in to what interventions are saving the most lives. Effectiveness estimates can also be obscured by how severity is defined. Even tracking who gets hospitalized can be a pretty coarse metric. Different hospitals use different criteria to admit patients, especially during surges, when capacity gets stretched. And parsing out the severity of an infection isn’t easy in someone who’s battling another ailment, says Westyn Branch-Elliman, an infectious-disease physician at VA Boston Healthcare System and Harvard Medical School. Nor are all serious COVID cases the same: Some people might be discharged after just a couple of days, while others end up on ventilators—nuances that get lost when all cases that meet the bare minimum criteria for “severity” are lumped together. Add to that the complexities of actual infections—which happen more commonly in the unvaccinated and layer on their own patinas of protection—and it’s that much tougher to figure out how well the shots are performing on their own. [Read: What COVID hospitalization numbers are missing] Our estimates are also always a few steps behind. The most up-to-date effectiveness numbers in the books still largely reflect how the shots are faring against BA.1, which, thanks to its speedier siblings, has now almost entirely blipped off the American map. If we’re having trouble figuring out where we stand on this mountainous trail, forking paths exacerbate the confusion, along with a compass that gets more challenging to calibrate by the day. Practically, that all makes assessing when, or whether, to intervene very difficult. A catastrophic, cliff-like plunge in effectiveness—especially one tied to the emergence of a new variant of concern—might prompt a scramble to revamp our vaccine recipes, stat. That doesn’t seem to be what we’re seeing, though, and experts are still working on timing our next steps just right. Scientists are used to strategizing against other viruses, such as the ones that cause seasonal flus: Scientists reformulate and readminister those shots every year, in an attempt to counteract both waning immunity and viral mutations before most people hit a winter surge. By comparison, this coronavirus’s spread is still too haphazard, too unpredictable. If we can barely gauge which mile marker we’re at, it’s hard to know how often we’ll need to update our approach. It has, at least, become clear that protection can fall off far faster in some vulnerable populations, who may need immune refurbishings more often: older people, immunocompromised people, people with certain chronic health conditions. In the rest of the population, though, the extent of the decline feels far murkier. Branch-Elliman told me that some studies are likely overestimating drops in effectiveness against severe disease: Some aren’t accounting for the immunity building up in the unvaccinated; others are failing to disentangle the true severity of infection in each case. Adjust for them, she said, “and the evidence for waning becomes much weaker.” Still, as the virus continues to change, and people’s most recent doses recede further into the past, “I think we are seeing a little bit” of a performance drop, says Huong McLean, an epidemiologist and a vaccine researcher at the Marshfield Clinic Research Institute. The dip isn’t massive—maybe a few percentage points over several months, in those who are up-to-date on their shots. “But,” Omer told me, “it is there.” The experts I spoke with couldn’t point to a single threshold at which they’d really start to worry—when the dreaded bottom of Protection Peak might feel just too close. One tentatively offered a dip below 50 percent effectiveness against severe disease as an obvious bad-news-bears benchmark. A couple said they’d start to worry at about 70 percent, while another told me that anything below the range of the 80s would “be clearly problematic” (which, maybe, means now). Martinez, of UNC Chapel Hill, framed it by outcomes: If rates of hospitalization or death among people up to date on their vaccines were to approach “an uncomfortably high rate”—maybe half what experts are seeing among the unvaccinated, he told me—“that’s when you want to patch this.” The clearest and most immediate intervention available would be administering an additional vaccine dose. And ideally, it would be tailored to better match the circulating strains du jour, which, for now, requires at least some nod to Omicron and its offshoots. Ellebedy suspects that the U.S. may be on track to revaccinate against this virus with a new vaccine recipe as often as each autumn, as we do for the flu—an annual adjustment that may become as necessary as redrawing trail maps to account for shifting mountain terrain. But it will be a behavioral hurdle as much as a technological one. Just a third of Americans are boosted, and uptake on future doses might not fare much better. [Read: The U.S. is about to make a big gamble on our next COVID winter] None of this means our vaccines have been a bust. “Protection against severe disease and death is what you want out of a vaccine in a public emergency—that’s the most important thing, and that’s what the vaccines have done,” Farber, the Columbia immunologist, told me. And the shots continue to trim down symptoms, transmission, and infection, even if they do not completely stave off those outcomes; the illnesses that do occur among the vaccinated also tend, on average, to be notedly less severe, Branch-Elliman points out. But our current crop of immunizations has its limits; shots won’t be enough to end the pandemic on their own, especially not with uptake lagging, and global vaccine equity still in a disastrous state. “I feel worried, just looking ahead,” Farber told me. “As long as the virus can infect, it’s going to change and adapt.” The virus could get more chances to transform into something more troubling; it may become even tougher to hold our ground against it, should we grow complacent now.
from https://ift.tt/feIX4kO Check out http://natthash.tumblr.com Pregnancy, in this age of modern medicine, comes with a series of routinely recommended prenatal tests: At 11 weeks, a blood draw and an ultrasound to check for conditions such as Down syndrome. At 15 weeks, another blood test, for anomalies such as spina bifida. At 18 to 22, an ultrasound anatomy scan of the baby’s heart, brain, lungs, bones, stomach, fingers, and toes. This is when many parents learn if they’re expecting a boy or girl—but the more pressing medical reason is to look for anatomical defects, including severe ones such as missing kidneys or missing parts of the brain and skull. With Roe v. Wade in place in America, women undergoing prenatal tests have typically had the legal right to end a pregnancy based on the information they learn. But abortion restrictions in certain states—by gestational age or by fetal anomaly—have already started limiting that choice. And if the Supreme Court overturns Roe, as seems likely, it will be further curtailed in some states. Routine parts of prenatal care could start to look quite different in states that ban abortion than in states that allow it. Even now, laws in more than a dozen states that restrict abortion past 20 weeks are changing the use of the second-trimester anatomy scans. “People are moving those tests backward, doing them earlier than is optimal,” says Laura Hercher, a genetic counselor at Sarah Lawrence College who recently conducted a survey of genetic counselors in abortion-restrictive states. But the earlier the scan, the less doctors can see. Certain brain structures, such as the cavum septum pellucidum, might not develop until week 20, says Chloe Zera, an obstetrician in Massachusetts. Being unable to find this structure could indicate a brain anomaly, or just that the scan was done too early. Doctors might also pick up evidence of a heart defect but not know how severe or fixable it is. At 20 weeks, the heart is only the size of a dime. [Read: The future of abortion in post-Roe America] Six states also currently restrict abortions on the basis of genetic anomalies. These laws typically target Down syndrome, or trisomy 21, in which the presence of a third chromosome 21 can have a range of physical and mental effects, milder in some children than others. Some states’ laws specifically mention Down syndrome; others extend the restrictions to a much wider range of genetic anomalies, many far more life-limiting than Down syndrome. In trisomy 13, for example, the physical anomalies are so severe that most babies live only for days or weeks. More than 90 percent do not survive past their first year. In states that currently restrict abortion based on genetic anomalies but still allow it for other reasons under Roe, patients can get an abortion if they do not mention the genetic anomaly. This puts doctors and genetic counselors in a bind. For instance, says Leilah Zahedi, a maternal-fetal-medicine physician in Tennessee, what if doctors see a severe heart defect on an ultrasound? The underlying cause of many such heart problems is Down syndrome. But Tennessee restricts abortions specifically on the basis of trisomy 21. Should doctors tell patients about the connection to Down syndrome? Should they do the genetic testing? It could help parents prepare for everything else that comes with Down syndrome. But it would make it harder for them to get an abortion, if they chose to have one. They would need to go to a different doctor who does not know about the diagnosis, and take care not to reveal it. Many of the current abortion restrictions do contain exemptions for cases with the most dramatic medical consequences: a fatal fetal anomaly or risk to the mother’s life. If Roe is overturned, many of the “trigger laws” that will immediately ban abortion in some states contain such exemptions as well. But what is “fatal” to the baby and what risk is acceptable to the mother are not entirely clear criteria. “There are very few bright lines in medicine,” says Cara Heuser, a maternal-fetal-medicine physician in Utah. “Laws really do not allow for all the nuance we see in medicine. They ignore the uncertainty.” When it comes to fetal anomalies, “it’s very rare we can say, ‘This is universally fatal,’” Zera told me. For example, in the case of a massive brain hemorrhage that destroys most of the brain tissue but leaves the brain stem intact, the baby can breathe at birth but will need other medical care. Does fatal mean fatal in the absence of certain medical interventions? Which ones? And does an anomaly have to be fatal immediately, or within some period after birth? [Read: When a right becomes a privilege] There is ambiguity in exceptions for the life of the mother, too. A genetic counselor in Texas told me about a recent patient whose fetus was triploid, meaning it had a complete extra set of 23 chromosomes. This is one of the universally lethal conditions. But triploidy also poses an extra risk to the mother, because these pregnancies are linked to preeclampsia, or dangerously high blood pressure. Texas currently restricts abortions past about six weeks except in “medical emergencies.” High blood pressure may not be an immediate medical emergency, but it can become one. “What’s scary about being a person who is pregnant in Texas,” says the genetic counselor, whom I agreed not to name because this person feared legal retribution in the state, is that many physicians will wait to provide treatment “until mom’s life is truly in danger.” The fetus will not survive, and delaying may only increase the risk to the mother, but “we have to wait until you get sick enough to deliver you.” These laws create a general climate where doctors who fear prosecution may hesitate to treat the mother. “Sometimes,” Heuser says, “that hesitation can be fatal.” If Roe is overturned and abortion is banned in many states, testing could take on a different role in prenatal care. Zahedi told me, anecdotally, of one recent patient whose doctor told her there wasn’t a point to genetic screening anymore. But she doesn’t actually think abortion bans will change the use of testing, even if they will limit what patients can do afterward. Most of her patients in Tennessee already do not choose abortion, she said, but the tests can provide information that inform obstetric care and prepare parents for what’s to come. Others brought up the possibility, in the long term, of insurance companies dropping coverage for prenatal tests. Cumulatively, “all of these types of screenings and tests are incredibly expensive,” Hercher, of Sarah Lawrence, told me. Insurance currently has a financial incentive to cover them because preventing the birth of a child with severe medical needs saves on costs down the line. But if abortion is illegal in many states, Hercher asks, will insurance companies, especially regional ones, want to continue covering these tests? Or will patients have to pay for them out of pocket? These tests are currently routine for pregnant women, but whether they stay that way in the future could depend on where you live and what you can afford. from https://ift.tt/TiGcNtp Check out http://natthash.tumblr.com Yesterday afternoon, I called the UCLA epidemiologist Anne Rimoin to ask about the European outbreak of monkeypox—a rare but potentially severe viral illness with dozens of confirmed or suspected cases in the United Kingdom, Spain, and Portugal. “If we see those clusters, given the amount of travel between the United States and Europe, I wouldn’t be surprised to see cases here,” Rimoin, who studies the disease, told me. Ten minutes later, she stopped mid-sentence to say that a colleague had just texted her a press release: “Massachusetts Public Health Officials Confirm Case of Monkeypox.” The virus behind monkeypox is a close relative of the one that caused smallpox but is less deadly and less transmissible, causing symptoms that include fever and a rash. Endemic to western and central Africa, it was first discovered in laboratory monkeys in 1958—hence the name—but the wild animals that harbor the virus are probably rodents. The virus occasionally spills over into humans, and such infections have become more common in recent decades. Rarely, monkeypox makes it to other continents, and when it does, outbreaks “are so small, they’re measured in single digits,” Thomas Inglesby, the director of the Johns Hopkins Center for Health Security, told me. The only significant American outbreak occurred in 2003, when a shipment of Ghanaian rodents spread the virus to prairie dogs in Illinois, which were sold as pets and infected up to 47 people, none fatally. Just last year, two travelers independently carried the virus to the U.S. from Nigeria but infected no one else. The current outbreaks in Europe and the U.S. are different and very concerning. The first case, which was identified in the United Kingdom on May 7, fit the traditional pattern: The individual had recently traveled to Nigeria. But several others hadn’t recently been to endemic countries, and some had had no obvious contact with people known to be infected. This suggests that the monkeypox virus may be surreptitiously spreading from person to person, with some number of undetected cases. (The incubation period between infection and symptoms is long, ranging from 5 to 21 days.) “It’s uncommon to see this number of cases in four countries at the same time,” Inglesby said. (The count may soon be seven: Since we spoke yesterday, monkeypox has been confirmed in Sweden and Italy, while Canada is investigating suspected cases.) These monkeypox outbreaks are also unique because … well … they’re occurring in the third year of a pandemic, “when the public is primed to be more acutely aware of outbreaks,” Boghuma Kabisen Titanji, a physician at Emory University, told me. “I don’t think that’s necessarily a good thing.” When it comes to epidemics, people tend to fight the last war. During the West African Ebola outbreak of 2014, American experts had to quell waves of undue paranoia, which likely contributed to the initial downplaying of the coronavirus. Now, because the U.S. catastrophically underestimated COVID, many Americans are panicking about monkeypox and reflexively distrusting any reassuring official statements. “I don’t think people should be freaking out at this stage,” Carl Bergstrom of the University of Washington told me, “but I don’t trust my own gut feelings anymore, because I’m so sick of all this shit that I tend to be optimistic.” Monkeypox, then, is a test of the lessons that the world has (or hasn’t) learned from COVID. Can we better thread the needle between panic and laxity, or will we once again eschew uncertainty in a frantic quest for answers that later prove to be wrong? To be clear, monkeypox isn’t COVID—they’re different diseases caused by different viruses with markedly different properties. COVID was completely unfamiliar when it first appeared, but monkeypox is a known quantity, and experts on the virus actually exist. One of them, Andrea McCollum of the CDC, told me that based on existing studies, monkeypox doesn’t spread easily, and not over long distances through the air. It transmits via contaminated surfaces or prolonged proximity with other people, which is why most outbreaks have been small, and why people have mostly transmitted the disease to either household members or health-care workers. “This isn’t a virus that, as far as we’re aware, would really take off in a population like COVID,” she said. “It really requires close contact for human-to-human transmission.” Of course, we have heard that before. In early 2020, many experts claimed that COVID spread only via contaminated surfaces or close-splashing droplets—hence the six-feet rules and hygiene theater. Now it is widely accepted that the disease spreads through smaller and farther-reaching aerosol particles—hence the importance of ventilation and masks. But that doesn’t mean history is repeating with monkeypox. A 2012 study suggested that the virus can persist in aerosols for several days—but that was under artificial laboratory conditions, and persistence is just one small part of the infection process. The fact remains that past monkeypox outbreaks have been inconsistent with a virus that travels as easily as the coronavirus. “Monkeypox does not scream ‘airborne’ at me; COVID-19 did,” Linsey Marr, an aerosol expert at Virginia Tech, told me. Then again, Marr is less certain about monkeypox than she was about COVID. And Titanji notes that our knowledge of monkeypox is based on just 1,500 or so recorded cases, as of 2018. “I’ve seen a lot of people writing as if everything we know about monkeypox is definitive and finalized, but the reality is that it is still a rare zoonotic infection,” she said. For that reason, “I’m in Team Cautious,” she said. “We can’t use what happened with previous monkeypox outbreaks to make sweeping statements. If we’ve learned anything from COVID, it’s to have humility.” For decades, a few scientists have voiced concerns that the monkeypox virus could have become better at infecting people—ironically because we eradicated its relative, smallpox, in the late 1970s. The smallpox vaccine incidentally protected against monkeypox. And when new generations were born into a world without either smallpox or smallpox-vaccination campaigns, they grew up vulnerable to monkeypox. In the Democratic Republic of Congo, this dwindling immunity meant that monkeypox infections increased 20-fold in the three decades after smallpox vanished, as Rimoin showed in 2010. That gives the virus more chances to evolve into a more transmissible pathogen in humans. To date, its R0—the average number of people who catch the disease from one infected person—has been less than 1, which means that outbreaks naturally peter out. But it could eventually evolve above that threshold, and cause more protracted epidemics, as Bergstrom simulated in 2003. “We saw monkeypox as a ticking time bomb,” he told me. This possibility casts a cloud of uncertainty over the current unusual outbreaks, which everyone I spoke with is concerned about. Are they the work of a new and more transmissible strain of monkeypox? Or are they simply the result of people traveling more after global COVID restrictions were lifted? Or could they be due to something else entirely? So far, the cases are more numerous than a normal monkeypox outbreak, but not so numerous as to suggest a radically different virus, Inglesby told me. But he also doesn’t have a clear explanation for the outbreak’s unusual patterns—nor does anyone else. Answers should come quickly, though. Within days, scientists should have sequenced the viruses from the current outbreaks, which will show whether they harbor mutations that might have changed their properties. Within weeks, European epidemiologists should have a clearer idea of how the existing cases began, and whether there are connections between them. As for the U.S., “there are currently no additional suspected cases” beyond the individual in Massachusetts, McCollum told me. But given the numbers in Europe, she’s standing by for more. The U.S. is, of course, in a better position with monkeypox than with COVID. Although the nation hadn’t planned for a coronavirus pandemic, it has spent decades thinking about how to handle smallpox bioterrorism. The two cases of monkeypox in 2021 provided handy test runs for those plans, which are now unfolding smoothly. For example, the case in Massachusetts was identified when the patient’s physician, having reviewed reports from the U.K., called the state’s public-health department on Tuesday. Within 12 hours, the department had collected and tested the patient’s samples. The next day, more samples arrived at the CDC, which confirmed monkeypox. “All of that worked really well,” McCollum said. “We’re a fairly well-oiled machine.” Also, there’s already a vaccine. One smallpox vaccine is 85 percent effective at preventing monkeypox and has already been licensed for use against the virus. And as another bioterrorism precaution, stockpiles of three smallpox vaccines are large enough “to vaccinate basically everyone in the U.S.” Inglesby said. And though monkeypox patients usually get just supportive care, a possible treatment does exist and has also been stockpiled: Tecovirimat, or TPOXX, was developed to treat smallpox but would likely work for monkeypox too. Monkeypox may also be less deadly than is frequently claimed. The oft-cited fatality rate of about 10 percent applies to a strain that infected people in the Congo Basin. The West African strain, which several of the current cases have been linked to, has a fatality rate closer to 1 percent—and that’s in poor, rural populations. “We haven’t seen fatalities in people who’ve had monkeypox in high-resource settings,” Rimoin said. Still, as COVID has shown, even when a disease doesn’t kill you, it can hardly count as “mild.” Monkeypox might not take off in the way that COVID did, but for those who get it, it remains a “substantial illness,” McCollum said. “If individuals are sick, they’re often sick for two to four weeks. It’s urgent to identify people early, get them treatment, and identify contacts.” It helps that one common symptom is an obvious rash, which looks like an extreme version of chickenpox. But unlike chickenpox, the monkeypox rash is usually preceded by a fever, the lesions are initially more painful than itchy, and the lymph nodes are often inflamed. “The constructive thing to do is to make sure that the public is aware of what monkeypox looks like,” Titanji said. For that reason, she added, it’s important to avoid stigmatizing infected people. Many of the current cases are in men who identify as gay, bisexual, or men who have sex with men—an unusual pattern not seen in previous monkeypox outbreaks. That has raised questions about a new route of transmission, but sex obviously involves prolonged close contact, which is how the virus normally spreads. As COVID showed, early narratives about a disease can rapidly and prematurely harden into accepted lore. And if those narratives turn into stigma, they could stop people from coming forward with symptoms. Communication might prove to be one of monkeypox’s hardest challenges, as it has been with COVID. “We need leaders who are saying, ‘Here’s what we know; here’s what we don’t know; we’ll find out; and we’ll be back tomorrow,’” Inglesby said. But some leaders have lost credibility during the recent pandemic, while others are being drowned out by armchair experts who have amassed large followings. “All of a sudden, everyone’s an expert in monkeypox,” Titanji said. from https://ift.tt/XYhsL5z Check out http://natthash.tumblr.com The baby-formula shortage has been something of a nightmare for Aleisha Velez, a 25-year-old mother of two who lives in Philadelphia. Velez relies on the federal government’s Woman, Infants, and Children (WIC) program to get free formula, which means she can’t just get the product shipped to her home. So over the past two months, she has called store after store to find in-stock formula before traveling up to an hour one-way on a train or a bus (or both) to get it. And then she does it all over again: Because many stores are limiting how much formula parents can buy, she now makes the trek about once a week, compared with once a month before the shortages. “I’m sitting here struggling to make sure my son has what he needs,” she told me while on the way back from a formula run. “I don’t see how it’s fair.” With more than 40 percent of the country’s infant formula currently out of stock, millions of parents are scrambling to get ahold of supplies. But other parents with the means and know-how are relying on a controversial workaround—they’re tapping into a black market that lets them get formula from around the world shipped right to their home. Across social media, parents have been swapping advice and resources for how to get hold of various kinds of European formula, which is illegal to import to the United States. Access to what is the primary form of nutrition for many babies has long been unequal. The parents of about 1.5 million infants have to wade through the aggravating bureaucracy of the welfare state simply to get a necessity. In contrast, 15 percent of parents evade the law to import European formula in order to access ingredients and nutrition standards that differ from what the FDA allows. American formula already is quite expensive, but smuggling in the European stuff is on another price tier altogether, running about four times more than the cheapest U.S. formula, and that’s before factoring in shipping costs. But now, as more wealthy parents opt for European-made formula in light of the crisis at home, the inequality is compounding. While some parents struggle to get formula at all, others are bypassing the American market to get what they view as superior formula delivered straight to their doorstep. [Read: We’ve never been good at feeding babies] The formula sold in the U.S. is highly regulated and provides adequate nutrition for growth, but skirting the law to buy products from Europe opens up a whole new world of options. Though no U.S. manufacturers make formula with goat milk, for example, which some parents say their babies tolerate better, several brands in Europe do. Because of all the different choices, the black market started gaining steam in about 2015 among parents who are hyper-focused on the ingredients their kids consume, Anthony Porto, a pediatric gastroenterologist at Yale who studies infant-feeding trends, told me. Indeed, on a prominent Facebook group with more than 30,000 members, parents write that they are looking for “the closest formula to breastmilk” and that they want to avoid “GMO ingredients” and “added corn syrup.” (The GMOs and corn syrup in American formulas haven’t been proven to be detrimental to babies.) They share notes and spreadsheets about the ingredients in formulas they consider “best,” including the Swiss brand Holle, the German brand HiPP, and the U.K. brand Kendamil. Because European brands aren’t out of stock, the latest bump in interest among Americans may have less to do with their ingredients than their availability. Though the Facebook group was created in 2016, the current shortages seem to have pulled even more people into this world. In recent days, the group seems to be full of posts from new members seeking guidance on switching to European formula. A representative of Happy Tots Organic, a website that sells European formula, said in an email that since news of the shortages began, “sales have increased by at least 25 to 30%,” and Organic’s Best, another website, noted that “we are receiving an exponential amount of orders.” But even for people with means, buying from the infant-formula black market is not necessarily straightforward. Parents can’t order directly from the European formula companies, or an online retailer like Amazon; they have to go through eBay, Facebook buying/selling groups, or third-party websites that sometimes get shut down. (In some cases, depending on where parents are purchasing European formula, they might not even know that it’s illegal.) And whereas U.S. formulas range from $0.50 to more than $1.90 per ounce, Holle’s goat-milk formula costs about $2.20 per ounce on the black market, not including shipping. The total cost can run close to $300 a month, if a baby is exclusively formula-fed. In Europe, these same formulas cost about a third of what they’re marked up to in the U.S. The potential problems go beyond just finding somewhere to buy European formula. In the past, the FDA has cracked down on the import of European formula by targeting the third-party websites that import and sell it online, and U.S. Customs seizes formula that it discovers at the border. (The FDA is now planning a process to temporarily allow in some formulas from abroad to alleviate the current shortage, provided they meet certain requirements.) Some safety concerns, too, make using European formula a bad idea, Porto said. The instructions typically aren’t in English, the preparation requires metric units, the ratio of water to powdered formula is different from the U.S. standard, and parents might not be alerted to recalls. There have been reports of parents mixing European formula wrong and giving their babies too little or too many calories as a result. Though Porto doesn’t recommend imported black-market European formula, he does appreciate that the European Union periodically updates their formula nutrition requirements based on current evidence, whereas the FDA has only made one change since 1985. For instance, in 2016, the EU added a requirement for DHA, which studies have indicated “improved kids’ outcome for verbal and nonverbal cognition,” he said, noting that many U.S. formulas contain less than half of the DHA amount required in Europe. (When I reached out to the FDA for comment on its infant-formula standards, a spokesperson declined, citing all the media inquiries that the agency is dealing with.) The black market couldn’t be more different from how families on WIC get baby formula. Each state runs its own WIC system, each with its own formula offerings. Even normally, WIC parents can access only a handful of options within a single brand, and, depending on the state, the formula they purchase must come from a brick-and-mortar store. Without a medical exemption, parents in South Carolina can select from three Gerber formulas; in Georgia, three from Enfamil. Even for states that are allowing WIC participants more choices than they normally do because of the shortage, that choice is unfortunately drastically limited by the current low availability. Parents want what’s best for their babies, and it of course makes sense that during a crisis they’re going to reach for whatever formula they can get, whatever the cost. Rich parents will always more easily access products for their babies—whether it’s self-rocking bassinets, chemical-free car seats, expensive baby food—but none is as essential to a baby’s first year of life as human milk or formula. The fundamental tragedy of this worsening inequality is that while rich parents can access European formula with higher levels of cognitive-enhancing DHA, for example, the parents who stand to gain the most from formula largely can’t. Lower-income parents are more likely to use formula than wealthier ones, because there are numerous barriers to breastfeeding for these families—such as no paid family leave and fewer lactation accommodations, says Ifeyinwa Asiodu, a professor at UC San Francisco whose research focuses on infant disparities. Now that formula has the nation’s attention, Porto hopes for changes that could ensure that formula access isn’t so skewed. Perhaps some of the changes that the FDA is now pursuing will become permanent, opening the door for European formulas that are legally transported and appropriately packaged for American consumers, which would also make them significantly cheaper and increase competition in our limited American-formula market. Or maybe states will ease up on their WIC restrictions, helping parents more easily purchase the formula they need or want. And changes to FDA regulations could ensure that every formula has the same minimum standards for helpful ingredients and harmful ones. For now, how American parents approach formula will continue to move in opposite directions. When I reached Velez on the bus, she lamented that at various points since the shortage began, she’s had to withhold bottles of formula and try to get her 9-month-old to eat more food now that he’s old enough for solids. And she was coming home without formula—the store she had visited was all out. The same week, a mom posted in the European-formula Facebook group with an update: “Just wanted to share that I ordered Kendamil on FormulaLand Inc and it got here in 4 days!” from https://ift.tt/kBFNDw9 Check out http://natthash.tumblr.com For weeks now, as COVID-19 cases have ticked upward in the Northeast and mid-Atlantic, pundits and political leaders have offered a supposedly reassuring refrain: Cases might be climbing, but hospitalizations aren’t yet following suit. In some places, that has been true. Several health-care workers around the country told me they’re seeing the lowest caseloads since last summer. A few aren’t having to treat COVID patients at all. Others are only seeing mildly sick people who need little more than IV fluids. “I don’t think there’s a huge amount of anxiety over what the next month might bring,” Debra Poutsiaka, an infectious-disease specialist at Tufts Medical Center, told me. “I could be wrong. I hope not.” The Biden administration shares those hopes: Having apparently given up on curtailing the coronavirus, it is counting on vaccines and treatments decoupling infection from severe illness enough to prevent the health-care system from becoming inundated again. The CDC’s current guidelines effectively say that Americans can act as if COVID is not a crisis—until hospitalizations reach a high enough threshold. The country still may be heading to that point. Hospitalizations are climbing in 43 states, especially in the Northeast. In Vermont, the rate of new admissions has already neared the peak of the recent Omicron surge. Earlier this month, “three different emergency-room docs said this is by far the worst that COVID has been at any point,” Tim Plante, an internist at the University of Vermont, told me. “They’re bewildered that it’s happening again.” Meanwhile, people in most of New York City are now advised to mask indoors again, after rising hospitalizations triggered the CDC’s “high” alert level. But even in calmer spots, Biden’s strategy overlooks a crucial truth: The health-care system is still in crisis mode. The ordeals of the past two years have tipped the system—and its people—into a chronic, cumulative state of overload that does not fully abate in the moments of respite between COVID waves. Some of the problems I’ve written about before: Even in quieter periods, health-care workers are scrambling to catch up with backlogs of work that went unaddressed during COVID surges, or patients who sat on health problems and are now much sicker. Those patients are more antagonistic; verbal and physical assaults are commonplace. Health-care workers can also still catch COVID, keeping them from their jobs, while surges elsewhere in the world create supply-chain issues that keep hospitals from running smoothly. All this, on top of two years of devastating COVID surges, means that health-care workers are so exhausted and burned out that those words have become euphemisms. In trying to describe his colleagues’ mental state, Plante brought up Migrant Mother—the famous photo from the journalist Dorothea Lange, which captured unimaginable hardships in a single haunting expression. “That look in her eyes is what I see in folks who’ve been on the front lines,” Plante told me. Enough health-care workers--nurses, in particular--have quit their jobs that even when hospitals aren’t deluged, the remaining workforce must care for an unreasonable number of patients over longer hours and more shifts. In a survey of nearly 12,000 nurses, conducted by the American Nurses Foundation this January, 89 percent said that their workplace was short-staffed, and half said the problem was serious. Worse, almost a quarter said that they were planning on leaving their jobs within the next six months, and another 30 percent said they might. Even if just a small fraction of them follow through on their intentions, their departure would heap more pressure upon a workforce that is already shouldering too much. “There’s a palpable concern that this can’t be our new normal,” Beth Wathen, president of the American Association of Critical-Care Nurses, told me. The problems are substantial and numerous enough that “if this moment was occurring without the horror of the moments that preceded it, we’d be shocked,” Lindsay Ryan, a physician at UC San Francisco, told me. “The calamity of the last years has numbed us to the calamity of the present moment.” America’s current pandemic strategy is predicated on the assumption that people can move on from COVID, trusting that the health-care system will be ready to hold the line. But that assumption is a fiction. Much of the system is still intolerably stressed, even in moments of apparent reprieve. And the CDC’s community guidelines are set such that by the time preventive actions are triggered, high levels of sickness and death will be locked in for the near future. For many health-care workers, their mental health and even their commitment to medicine are balanced on a precipice; any further surges will tip more of them over. “I feel like I’m holding on by a thread,” Marina Del Rios, an emergency physician at the University of Iowa, told me. “Every time I hear a new subvariant is coming along, I think: Okay, here we go.” During the Omicron surge, Kelley Cabrera, a nurse based in New York, watched three patients die in a single shift. While zipping another in a body bag, “something in me broke,” she told me. “I told my friend, 'I cannot do another shift like this again.’” She couldn’t sleep; when she did, she had nightmares about work. Once the surge abated, she quit her job, and now does short-term travel contracts. “When we’re in the middle of a trauma, our brain has this incredible capacity to go into survival mode," Mona Masood, a psychiatrist who founded a support line for physicians, told me. "It’s only afterward, when we let go of that, that there’s this surge of grief, sorrow, anxiety, and fear.” In those moments of calm, many health-care workers decide they’ve had enough. The resulting staff shortages are especially acute in rural areas. Kelly McGrath, a chief medical officer in Idaho, told me that the two hospitals where he works will have lost eight of their 20 physicians by the end of the summer—and despite intense efforts, he has struggled to replace any of them. Meanwhile, one of the hospitals normally has a full staff of 13 registered nurses and has turned over 21 since the pandemic began. And the hospitals still have to care for about 28,000 people spread across an area the size of Massachusetts. “Workforce was always a challenge in rural health care, but we’ve gone from a challenge to a crisis,” McGrath told me. “I’ve never seen anything like it.” COVID itself depletes the depleted workforce further by periodically taking out waves of health-care workers. Being vaccinated, those workers mostly incur mild or moderate symptoms, but must nonetheless stay away from medically vulnerable patients. (Mild infections can still put them at risk of long COVID, too.) This means that COVID can still hammer the health-care system even without sending a single person to the hospital. “The choice to lift all restrictions means that anyone who lives in the community will get COVID more—and that includes the workforce that takes care of patients,” Kathleen McFadden, a chief resident at Massachusetts General Hospital, told me. She had just recovered from a bout of COVID, during which already stressed colleagues had to fill in for her. 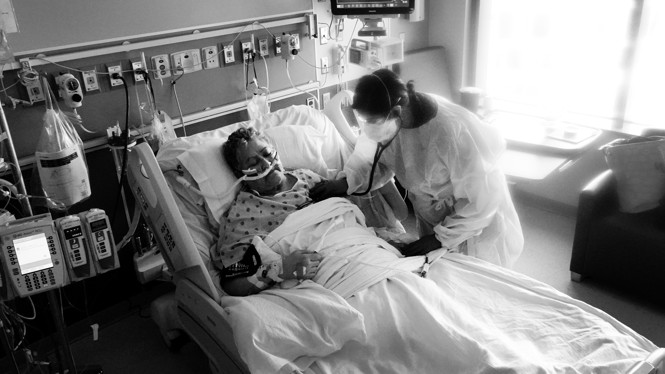
Even when missing people can be replaced, missing knowledge cannot. The pandemic pushed many veteran health-care workers into early retirement, lowering the average experience level in American hospitals. “I don’t think the public really understands how great the loss of this generational knowledge is,” Cabrera told me. In her current job, she had just six weeks of orientation, which she describes as “shockingly short,” from some people who had been in the ER for less than a year. When inexperienced recruits are trained by inexperienced staff, the knowledge deficit deepens, and not just in terms of medical procedures. The system has also lost indispensable social savvy—how to question an inappropriate decision, or recognize when you’re out of your depth—that acts as a safeguard against medical mistakes. And with established teams now ruptured by resignations, many health-care workers no longer know—or trust—the people at their side. “In an industry where our communication has to be spot-on and effective, that’s a setup for unsafe conditions,” Lisa Zegan, a patient safety officer based in Maryland, told me. The health-care workers who’ve stayed in their jobs also face several long-term problems that the pandemic exacerbated. Hospitals still depend on a just-in-time economy, and brittle international supply chains that regularly snap in the COVID era. The Shanghai lockdown precipitated a global shortage of contrast fluids, which are used in medical imaging like CT scans and MRIs; hospitals are postponing scans and the surgeries that depend on them. “We get shortage emails popping up all the time, and I never used to get these,” Lindsay Ryan told me. Hours before we spoke, she got an email warning of a crucial shortage of concentrated saline—essentially super-salt, which is used to treat severe electrolyte abnormalities. “When you need it, you need it,” Ryan said. These staffing and supply problems are all happening at a time when “our hospital capacity is running high due to folks catching up on care and other needs,” Nathan Chomilo, a pediatrician and health-care leader based in Minnesota, told me. And now, in some places, flu and other respiratory viruses that had been almost completely suppressed by widespread masking are back in force. People who were infected with COVID in past surges are returning with heart failure, diabetes, respiratory problems, and lingering symptoms of long COVID. Absurdly, it’s often hard to get people out of the hospital, Sara Wolfson, a geriatrician at Nebraska Medicine, told me. Many elderly patients still need care after they’ve stabilized, but it’s hard to discharge them, because long-term care facilities and home-health agencies are also incredibly short-staffed and unable to accommodate new patients. Some people in Wolfson’s care have ended up staying in the hospital for 40 to 45 days longer than they needed to. These logjams take up beds that are needed for elective surgeries, which hurts a hospital’s bottom line. And such deficits will become more consequential as emergency COVID funding dries up. “Some people may look at the funds as welfare for hospitals, but that money was key to keeping our staff whole while we took big losses,” McGrath told me. Health-care workers are still providing the best care they can possibly give. But the limits of their best have been severely constrained by a medical system that was stretched thin well before COVID arrived and has been diminished with every surge since. This compounds exhaustion with moral injury—the distress that comes from knowing what good care looks like and being unable to provide it. And when things go wrong, “the hospital isn’t coming in to apologize to patients,” Cabrera said. “We apologize. We face the brunt of everything.” At the same time they are struggling to provide care, they must also handle, for example, people who are annoyed to find hospitals still enforcing visitation rules to protect vulnerable patients. “We’re dealing with very angry people: I don’t understand, the pandemic’s over, I don’t have to wear a mask,” Wolfson told me. “It piles onto the exhaustion. You get tired of explaining.” Each fresh challenge layers upon the cumulative bedrock of two traumatic years. Every time McFadden passes a particular room in her hospital, she is yanked back to the spring of 2021. She remembers a patient saying “I’m really, really scared, Kathleen” before having every possible bad complication of COVID and lapsing into a coma from which she has still not awoken. Those words feel like they’re still echoing in the walls of McFadden’s workplace. “That’s one of maybe 50 stories I could tell you,” she said. “I walk past those rooms and relive those memories. The rest of the world has moved on, but you can’t simply move on from your profession turning into trauma day after day.” These problems are not obvious when looking at bed-occupancy charts or hospitalization curves. The entire health-care system has effectively developed a chronic illness. Its debilitating symptoms are persisting long after its initial acute sickness and affecting every part of its body. And because they are invisible to the outside, they are easy to dismiss. They aren’t accounted for in the calculations that are supposed to keep the country from hurtling back into another, unmanageable bout with COVID. Health-care workers sometimes feel as if they are living in a different world from those around them. Through the pandemic, they have wrestled with the gulf between the horrors they saw in their workplaces and the casual attitudes they beheld outside. For many, that cognitive dissonance is greater than ever. The relentless surges locked them in a two-year dystopian stasis, from which they are emerging to find that their old lives are unrecognizable. Many callers to Mona Masood’s physician support line have talked about lost friendships and imminent divorces. “We were holding back this wall, and it gave everyone a chance to keep going and get through,” Masood said. But that created a chasm between health-care workers and the rest of society—a pattern that Masood also hears among veterans returning from war. “I feel distanced from my outside-of-hospital friendships,” Marina Del Rios told me. 
Some health-care workers have turned toward one another, finding solace in the camaraderie that comes from facing trauma together. “For those that remain, there’s that band-of-brothers-and-sisters feeling,” McGrath told me. Others doubled down on the idealistic sense of mission that first got them into medicine. McFadden feels less burned out on days when she spends more time at patients’ bedsides, rather than staring at electronic medical records. “Making other people feel human in the hospital reminds me of the humanity still deep inside me,” she recently tweeted. But for a third group, the only way out is to pull away—by quitting, moving to less stressful roles, or shifting to temporary work. “I was putting so many other people’s needs ahead of my own, which is what nurses tend to do,” Cabrera told me. But eventually, “there was this realization: I don’t have to be this miserable.” Worryingly, this group includes much of health care’s next generation. In the American Nurses Foundation’s recent survey, nurses under 35 were twice as likely to report burnout as those over 55, and more likely to be planning on quitting. Many hospitals are now facing an unenviable bind. Without chances to recover from the past two years, more people will leave, and the staffing crisis will deepen. But for many people, recovery means doing less—at a time when institutions need their workers to do more. “For health-care workers, that’s not our problem; that’s the system’s problem,” Masood told me. “When you say burnout, you’re blaming people for feeling a very normal outcome of being put in a situation that’s depleting us of our energy and humanity. When a house catches fire, we don’t say it was burned out. We say it was burned down, and then we look for the source.” For too long, the U.S. has relied on the “individual grit” of its health-care workers, Jennifer Sullivan, who runs strategic operations for the south's Atrium Health system told me. Its challenge, now, is to create a health-care system that’s as resilient as the people in it have been forced to be. from https://ift.tt/APVIGt8 Check out http://natthash.tumblr.com Sudden infant death syndrome, or SIDS, “will be a thing of the past,” according to Carmel Harrington, a sleep researcher at the Children’s Hospital at Westmead, in Australia. A press release describes her new study, out this month, as a “game-changing” effort and a “world-first breakthrough” that could prevent future deaths from the tragic illness. Celebrations quickly spread on social media: “THEY FOUND THE CAUSE OF SIDS. Excuse me while I cry for all the parents,” one viral tweet declared. “Closest thing to a miracle in a long time,” said another. The press soon picked up the story. On Friday, a segment on Good Morning America touted Harrington’s “very, very important study” of SIDS, while a story in the New York Post promised that her data would “bring closure to countless parents who have endured the nightmare of losing a child.”
Sadly, these claims are quite absurd. The original research paper, published on May 6, described a small-scale but interesting project: Harrington and her colleagues measured activity levels of a protein called butyrylcholinesterase in dried blood collected from about 600 babies shortly after birth, including 26 who died from SIDS and 30 who went on to die from a different condition during their first two years of life. On average, those who died from SIDS had somewhat less butyrylcholinesterase activity in their blood than healthy newborns did. According to the study’s authors, this suggests that, with further work, the protein “could potentially be used as a biomarker to identify and prevent future SIDS deaths.” If that qualifies as a scientific “miracle,” the bar is inches from the ground. Even after decades of research, SIDS remains “unexpected, dramatic, and devastating,” as three prominent doctors put it in a New England Journal of Medicine editorial published over the weekend. If researchers had really pinpointed a biological cause for these deaths—as some press reports have claimed—it would salve parents’ anxiety and might lead to future treatments. But one need only read the new paper in its entirety to see they haven’t reached this goal. At best, the study represents an incremental advance. This is not meant to be an insult; science works in increments. But the numbers don’t suggest that a screening test for SIDS is really in the works, let alone one that will quickly end the scourge of infant deaths. The authors report that protein-activity levels were measured in a range of 1.7 to 23.3 units per milligram for healthy newborns, and from 2.9 to 10.8 for those who died of SIDS. Though the group averages were different overall (7.7 versus 5.6), individual values still overlapped a great deal. In other words, a low protein-activity level at birth could be found in a baby who might end up dying from SIDS, as well as one who would go on to live a healthy life. I reached out to Harrington and her co-author Karen Waters, a professor of child and adolescent health at the Children’s Hospital at Westmead, to ask about this issue, among others. Measuring the protein “will not work as a universal screening test, for precisely the reasons that you have highlighted,” Waters told me via email. Harrington said that their “finding represents the possibility for the future identification of infants at risk for SIDS” and that the study identifies “a measurable biochemical marker (not cause)” of the condition. The confusing and controversial status of SIDS as a formal diagnosis adds to the uncertainty. SIDS is considered a “diagnosis of exclusion,” which means that it applies only when other causes have been carefully ruled out, and also that it is likely to comprise a number of different conditions. Some forensic pathologists have abandoned the diagnosis entirely on account of this ambiguity, James Gill, the chief medical examiner of Connecticut, told me. The authors of this month’s study did not have access to autopsy details for any of their subjects, and relied in most cases on a coroner’s assessment that SIDS had been the cause of death. Even if it were possible to develop a screening test for SIDS, we might not want to use it. As a hospital pathologist myself—which is to say, as a doctor who specializes in diagnostic testing—I know that every form of screening makes mistakes. Sometimes, the benefits from these tools are worth the harm of an occasional error. Cervical-cancer screening, for example, greatly reduces deaths even though pap smears regularly lead to unhelpful results. But a wonky SIDS test would have catastrophic ill effects. A false positive result would terrify new parents. A false negative could lead them to abandon safe-sleeping practices—or far worse, make them seem at fault if SIDS did strike. Even true results might not be much help, because early-detection tests are only as good as the treatments we use in response to them. An aggressive campaign by pediatricians to promote safer sleep practices has caused the number of SIDS deaths to plummet since the 1990s. That campaign’s advice is already given out to everyone, and would not change on the basis of a blood test. [Read: Get ready for a wave of missed infections] Given that no further interventions would be available for infants flagged as high-risk by a screening test for SIDS, I asked the authors whether it makes sense to measure babies in this way. Waters responded by citing the “fundamental principle” that you should not screen newborns for disease unless you can “affect the outcome for the child.” Harrington has suggested in an interview that the researchers “don’t know the shape of what the intervention will be at this stage.” If the study’s findings were ambiguous, and its implications dubious, why did the research get so much attention in the media? Many outlets seemed impressed by its connection to The Lancet, founded in 1823, and one the world’s most prestigious medical journals. The SIDS paper did not actually appear in The Lancet, but rather in a lesser-known periodical called eBioMedicine, which happens to be published under The Lancet’s umbrella brand (along with more than 20 other journals). Media coverage glossed over that distinction, though, or ignored it altogether. (Good Morning America managed to combine the two journals’ names into a fictional publication called “eLancet.”) These errors are understandable; prominent Lancet branding on eBioMedicine’s website and web address make it easy to get confused, and journal editors sometimes take advantage of academic prestige to court media attention. The study’s tenuous connection to The Lancet was just one small part of its appeal. More significant was Harrington’s own story: She’d lost her son to SIDS 29 years ago, and then watched as a friend lost a baby to the same ailment a few years later. Harrington spent the intervening decades trying to discover a way to prevent this tragedy for others. “I made a solemn resolution there and then to leave no stone unturned in my quest to solve the mystery of the Sudden Infant Death Syndrome,” she wrote in a request to crowdfund her research that was first posted in August 2018. Before the study was published this month, the campaign hadn’t received a contribution since 2019; now donations have been pouring in. As of yesterday, the campaign had raised about $50,000, mostly in small increments. “Since we have published our research, I have continued to be overwhelmed by the generosity of the community,” Harrington told me. There’s no shame in soliciting funds for a good cause, and Harrington’s scrappy effort to keep her research going could be seen to merit praise. But Harrington herself has linked improbable claims about the science to overt requests for money: “To get us there, we need a lot of funding,” she told an interviewer, moments after saying that she “knows” that SIDS will be eradicated in “three to five years’ time.” (The hospital, which manages the endeavor’s charitable account, lent credence to this accelerated time frame in its press release.) An article from the Australian Broadcasting Corporation quoted Harrington making a plea for further backing: “We know what we have to do. It’s just actually getting the funding for it.” But the story, like numerous others, did not provide any appraisal of the research from independent experts, which would have helped inform potential donors. Harrington, in her email to me, reiterated her claim that screening tests and interventions “could be 3-5 years away” with appropriate funding. Many outlets also neglected to mention the study’s known limitations, as described in the paper. In that context, the authors acknowledge that they examined relatively few subjects, and that the tested blood was more than two years old. Their results could, therefore, turn out quite differently if the technique were put into widespread practice. “There is a lot more work to be done before this can be heralded as a solution,” Waters told me in her email. “As we said in the paper, it offers new directions for research in the field.” Harrington told me that “this finding is only one bit of the puzzle and there is so much more to learn.” Harrington’s personal accomplishments cannot be dismissed, even if new tests and treatments seem further away than she claims. Most of us never generate a speck of new scientific knowledge. To come back from tragedy, toil for decades, and then produce a promising approach for closer study … well, that may not be miraculous, but it matters all the same. from https://ift.tt/hSZN0Wq Check out http://natthash.tumblr.com |
Authorhttp://natthash.tumblr.com Archives
April 2023
Categories |
 RSS Feed
RSS Feed
